"Opposite Behaviors" of Macrophages Unsolved Problems Nov. 29, 2017
(Movements or responses that are the opposite of all other differentiated cell types)#1) On gradients of hydrophilic versus hydrophobic materials, nearly all tissue culture cells move onto the more hydrophilic surface (glass in preference to metal; metal in preference to cellulose acetate). But macrophages move onto more hydrophobic surfaces, in preference to hydrophilic.
#2) In voltage gradients, macrophages (and osteoclasts) move toward the positive electrode; Fibroblasts line up perpendicular to the gradient, and fish epidermal cells move toward the negative electrode (but if exposed to some ionophores will reorient toward the positive electrode!)
#3) Proteolytic enzymes ("trypsin" meaning impure mixtures of pancreatic enzymes) and calcium chelators (usually EDTA) cause most tissue culture cells to round up, and are routinely used to transfer cell populations from one dish to another.
Macrophages differ in not rounding up when treated with trypsin or EDTA.
If anything, macrophages increase spreading in response to trypsin.
#4) Roughened polystyrene somehow inhibits spreading of every kind of cell except macrophages, whose spreading is favored by roughening. Macrophages will run along scratched lines like trains on a track; but other cells stop at the edges of scratches.
#5) Although most cells are inhibited from crawling under or over each other, macrophages are somehow stimulated to accumulate underneath mesenchymal cells.
---------------------------------------------------------------------------------------
The photograph in the Wikipedia article about macrophages looks nothing like an actual macrophage. On the other hand, the two videos near the end of this article really do show actual macrophages. At least 14 different names are used to refer to macrophages depending on their location and/or origin in different parts of the body.
Wikipedia article on mononuclear phagocyte system
Although the Greek root "macro" means "big", macrophages are one of the smallest differentiated cell types in the body. However, they can phagocytize larger objects.
---------------------------------------------------------------------------------------
Evidence for a Monoclonal Origin of Human Atherosclerotic Plaques
PNAS 1973: volume 70(6), pp. 1753-1756 Earl P. Benditt and John M. Benditt, Dept. of Pathology, University of Washington School of Medicine, Seattle WA 98195
Abstract: The main cellular elements of atherosclerotic plaques are smooth muscle cells. Because these plaques differ from their precursors in the underlying artery wall in several ways, we have asked the question: Are human atherosclerotic plaques polyclonal or monoclonal in their origin? The X-linked glucose-6-phosphate dehydrogenase (EC 1.1.1.49) in heterozygotic females has been used to obtain an answer. 30 Plaques of different degrees of complexity and 59 samples of normal aorta and iliac artery walls from four females, 25-79 years old, were investigated. The data show that fibrous caps even of relatively large atheromatous plaques, 0.5 cm or greater in diameter, are composed of cells that produce solely or predominantly one enzyme type, whereas samples of artery wall media and intima as small as 0.1 mm3 are regularly composed of a mixture of cell types. If plaques were a response to injury akin to a healing wound, a reaction to a growth stimulant, or formed due to an organization of a mural thrombus, they would be expected to be polyclonal. Hence, the results imply that atherosclerotic plaques in human beings arise by another mechanism. The mechanism compatible with the monoclonal nature of atherosclerotic plaques is mutation, and the likely causes are chemical mutagens or viruses.
---------------------------------------------------------------------------------------
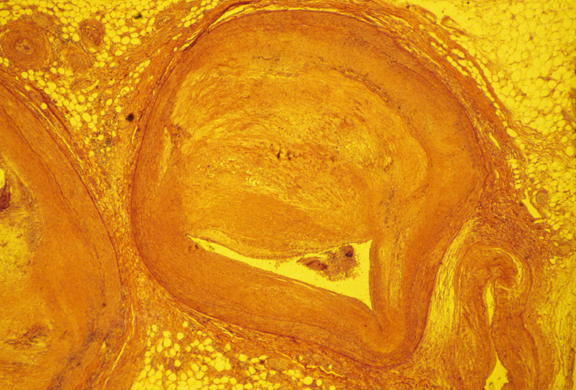
Photograph of a cross section of atherosclerotic artery.